Gynecological Cancer
Gynecological cancers are a group of malignancies that affect the female reproductive system, including the ovaries, uterus, cervix, vagina, and vulva. These cancers can develop silently, often showing subtle symptoms such as abnormal bleeding, pelvic pain, bloating, or unexplained weight loss. Early detection through routine screenings like Pap smears, HPV testing, ultrasounds, and blood markers is critical for effective treatment and improved survival rates. Women are encouraged to undergo regular check-ups and be aware of changes in their reproductive health.
Treatment for gynecological cancers depends on the type, stage, and overall health of the patient. Surgical removal of tumors is often combined with chemotherapy, radiation therapy, or targeted therapies to achieve the best outcomes. Multidisciplinary care involving gynecologic oncologists, surgeons, and medical and radiation specialists ensures personalized treatment plans. Preventive measures, including HPV vaccination, healthy lifestyle choices, and timely medical consultation, can significantly reduce risks and improve long-term health.
Types of Gynecological Cancers Treated by Dr. Harish Ravoori
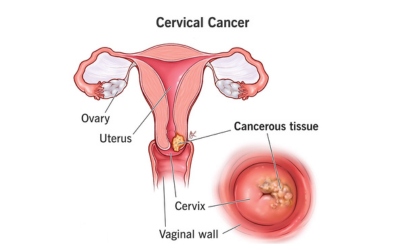
Cervical Cancer
Caused by HPV, this cancer of the cervix is preventable with screening and vaccination. Early treatment from a seasoned cervical cancer specialist with the appropriate intervention can make a life-changing difference.
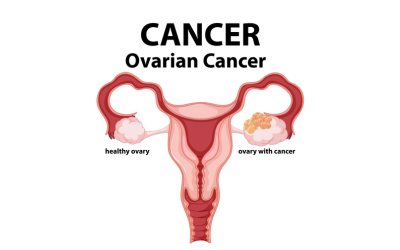
Ovarian Cancer
Characterized by vague symptoms, this cancer begins in the ovaries and most times needs surgery as well as chemotherapy.
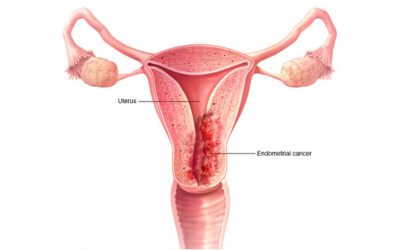
Uterine (Endometrial) Cancer
Usually occurs in postmenopausal women. Advanced treatment strives to maintain as much function and fertility as possible.
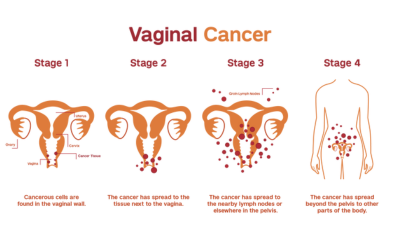
Vaginal Cancer
A serious, though uncommon, type of cancer on the vaginal walls—handled well with precision surgery.
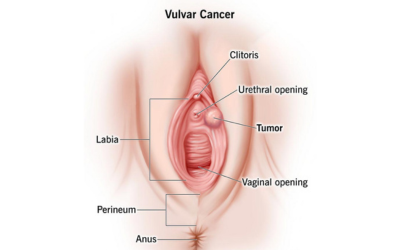
Vulvar Cancer
Usually diagnosed through abnormal itching or skin changes. Needs to be treated with careful surgical removal, sometimes aided by reconstructive assistance.
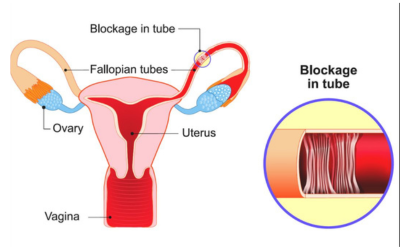
Fallopian Tube Cancer
Rare and often confused with ovarian cancer. Accurate diagnosis and treatment are key.
Diagnosis & Staging
Accurate diagnosis is the foundation of effective treatment—and it starts with the right steps.

Pelvic Examination
A manual check of the uterus, cervix, and ovaries to feel for any unusual growths or abnormalities.
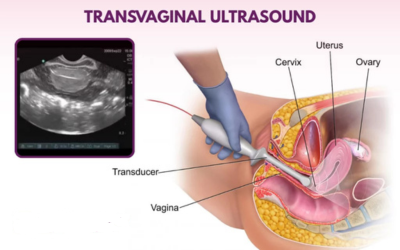
Ultrasound & Transvaginal Scans
These imaging studies yield a good visual of reproductive organs to detect cysts, tumors, or fluid accumulation.
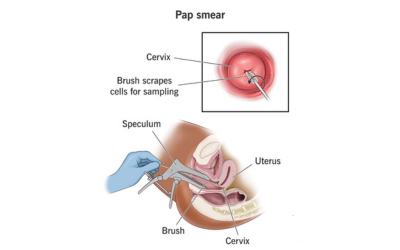
Pap Smear & HPV Testing
To identify abnormal cells of the cervix or high-risk HPV types prior to cancer formation.
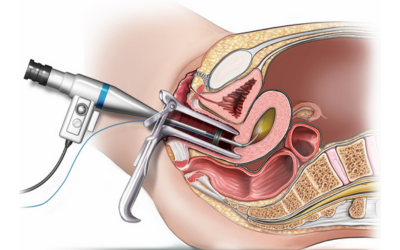
Endometrial Biopsy
A uterine lining sample is taken to confirm or rule out endometrial (uterine) cancer.
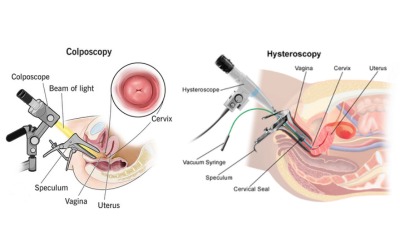
Colposcopy & Hysteroscopy
Both enable direct visualization of the cervix and uterine cavity with the ability to perform targeted tissue sampling if indicated.
MRI / CT / PET Scans
These examinations provide highly detailed, cross-sectional views of organs and assist in determining the extent of spread of the cancer.
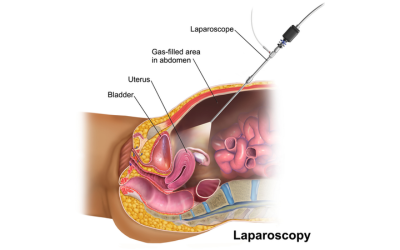
Laparoscopy
A procedure with minimal invasiveness that provides a good view of the pelvic and abdominal cavity—usually for diagnosis, staging, or biopsy.
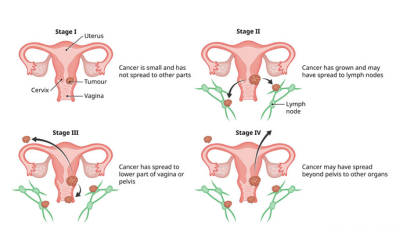
Cancer Staging (I–IV)
Each stage defines how far the cancer has developed—from being within the original organ (Stage I) to extending to distant organs (Stage IV).
Frequently asked questions
Cervical cancer is the most commonly diagnosed gynecological cancer, especially in developing countries like India.
Yes—regular screenings, HPV vaccination, and healthy lifestyle choices can significantly reduce the risk of several types.
In most situations, yes. Fertility-preserving surgeries and fertility-sparing treatments are available depending on the stage and type of cancer.
Yes. Postmenopausal women are actually more prone to cancers like endometrial and vaginal cancer.

